Leukemia
Leukemia
What is Leukemia
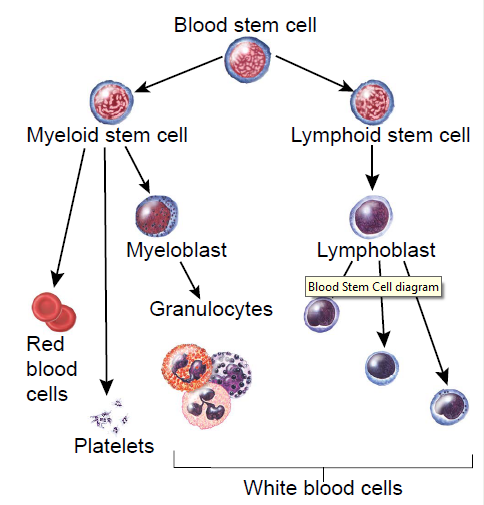
In a person with leukemia, the bone marrow produces abnormal white blood cells that are called leukemia cells and leukemic blast cells. The abnormal cells can’t produce normal white blood cells.
Leukemia cells divide to produce copies of themselves. The copies divide again and again, producing more and more leukemia cells.
Unlike normal blood cells, leukemia cells don’t die when they become old or damaged. Because they don’t die, leukemia cells can build up and crowd out normal blood cells. The low level of normal blood cells can make it harder for the body to get oxygen to the tissues, control bleeding, or fight infections.
Also, leukemia cells can spread to other organs, such as the lymph nodes, spleen, and brain.
Types of Leukemia
Lab tests help the doctor find out the type of leukemia that you have. For each type of leukemia, the treatment plan is different.
Acute and Chronic Leukemias
Leukemias are named for how quickly the disease develops and gets worse:
Acute: Acute leukemia usually develops quickly. The number of leukemia cells increases rapidly, and these abnormal cells don’t do the work of normal white blood cells. A bone marrow test may show a high level of leukemia cells and low levels of normal blood cells. People with acute leukemia may feel very tired, bruise easily, and get infections often.
Chronic leukemia
Chronic leukemia usually develops slowly. The leukemia cells work almost as well as normal white blood cells. People may not feel sick at first, and the first sign of illness may be abnormal results on a routine blood test. For example, a blood test may show a high level of leukemia cells. If not treated, the leukemia cells may later crowd out normal blood cells.
Myeloid and Lymphoid Leukemias
Leukemias are also named for the type of white blood cell that is affected:
Myeloid: Leukemia that starts in myeloid cells is called myeloid, myelogenous, or myeloblastic leukemia.
Lymphoid: Leukemia that starts in lymphoid cells is called lymphoid, lymphoblastic, or lymphocyticleukemia. Lymphoid leukemia cells may collect in the lymph nodes, which become swollen.
Molecular classification
Risk factor of Leukemia
Radiation
Large doses of Sr-90 emission from nuclear reactors, nicknamed bone seeker increases the risk of bone cancer and leukemia in animals, and is presumed to do so in people.
Genetic conditions
Some people have a genetic predisposition towards developing leukemia. This predisposition is demonstrated by family histories and twin studies. The affected people may have a single gene or multiple genes in common. In some cases, families tend to develop the same kinds of leukemia as other members; in other families, affected people may develop different forms of leukemia or related blood cancers.
In addition to these genetic issues, people with chromosomal abnormalities or certain other genetic conditions have a greater risk of leukemia. For example, people with Down syndrome have a significantly increased risk of developing forms of acute leukemia (especially acute myeloid leukemia), and Fanconi anemia is a risk factor for developing acute myeloid leukemia. Mutation inSPRED1 gene has been associated with a predisposition to childhood leukemia.
Chronic myelogenous leukemia is associated with a genetic abnormality called the Philadelphia translocation; 95% of people with CML carry the Philadelphia mutation, although this is not exclusive to CML and can be observed in people with other types of leukemia.
Non-ionizing radiation
Whether or not non-ionizing radiation causes leukemia has been studied for several decades. The International Agency for Research on Cancer expert working group undertook a detailed review of all data on static and extremely low frequency electromagnetic energy, which occurs naturally and in association with the generation, transmission, and use of electrical power. They concluded that there is limited evidence that high levels of ELF magnetic (but not electric) fields might cause some cases of childhood leukemia.[43] No evidence for a relationship to leukemia or another form of malignancy in adults has been demonstrated. Since exposure to such levels of ELFs is relatively uncommon, the World Health Organization concludes that ELF exposure, if later proven to be causative, would account for just 100 to 2400 cases worldwide each year, representing 0.2 to 4.9% of the total incidence of childhood leukemia for that year (about 0.03 to 0.9% of all leukemias).
Symptoms of Leukemia
The most common symptoms in children are easy bruising, pale skin, fever, and an enlarged spleen or liver.
Damage to the bone marrow, by way of displacing the normal bone marrow cells with higher numbers of immature white blood cells, results in a lack of blood platelets, which are important in the blood clotting process. This means people with leukemia may easily become bruised, bleed excessively, or develop pinprick bleeds (petechiae).
White blood cells, which are involved in fighting pathogens, may be suppressed or dysfunctional. This could cause the patient's immune system to be unable to fight off a simple infection or to start attacking other body cells. Because leukemia prevents the immune system from working normally, some patients experience frequent infection, ranging from infected tonsils, sores in the mouth, or diarrhea to life-threatening pneumonia or opportunistic infections.
Finally, the red blood cell deficiency leads to anemia, which may cause dyspnea and pallor.
Some patients experience other symptoms, such as feeling sick, having fevers, chills, night sweats, feeling fatigued and other flu-like symptoms. Some patients experience nausea or a feeling of fullness due to an enlarged liver and spleen; this can result in unintentional weight loss. Blasts affected by the disease may come together and become swollen in the liver or in the lymph nodes causing pain and leading to nausea.
Diagnosis & Tests
Diagnosis is usually based on repeated complete blood counts and a bone marrow examination following observations of the symptoms. Sometimes, blood tests may not show that a person has leukemia, especially in the early stages of the disease or during remission. A lymph node biopsy can be performed to diagnose certain types of leukemia in certain situations.
Following diagnosis, blood chemistry tests can be used to determine the degree of liver and kidney damage or the effects of chemotherapy on the patient. When concerns arise about other damage due to leukemia, doctors may use an X-ray, MRI, or ultrasound. These can potentially show leukemia's effects on such body parts as bones (X-ray), the brain (MRI), or the kidneys, spleen, and liver (ultrasound). CT scans can be used to check lymph nodes in the chest, though this is uncommon.
Despite the use of these methods to diagnose whether or not a patient has leukemia, many people have not been diagnosed because many of the symptoms are vague, non-specific, and can refer to other diseases. For this reason, the American Cancer Society estimates that at least one-fifth of the people with leukemia have not yet been diagnosed.
Treatment
The treatment that’s right for you depends mainly on the type of leukemia, your age, and your general health. People with leukemia have many treatment options, and you may receive more than one type of treatment.
Treatment options may include:
Watchful waiting
Your doctor may suggest watchful waiting if you’re diagnosed with chronic lymphocytic leukemia (CLL) but you don’t have symptoms. Watchful waiting means delaying treatment until you have symptoms. The purpose is to avoid the side effects of treatment as long as possible.
If you and your doctor agree that watchful waiting is a good idea, you’ll get exams and blood tests every 3 to 6 months. Your doctor may suggest starting treatment if you develop symptoms.
Chemotherapy
Most people with leukemia are treated with chemotherapy. Chemotherapy uses drugs to kill leukemia cells.
Several drugs are used for leukemia, and they may be given in different ways. The drugs used for leukemia may be given through a thin needle directly into a vein (intravenously) and as pills and liquids that you swallow. The drugs enter the bloodstream and can kill leukemia cells almost all over the body.
However, many drugs given directly into a vein or taken by mouth can’t pass through the tightly packed blood vessel walls found in the brain and spinal cord. If leukemia affects the brain or spinal cord, the drugs may be given through a needle into the fluid that fills the spaces in and around the brain and spinal cord. This method is known as intrathecal chemotherapy, and it’s given in two ways:
- item__Into the spinal fluid: The doctor may inject drugs into the spinal fluid. Injections into the spinal fluid can be painful.
- item__Under the scalp: The surgeon may place a device known as an Ommaya reservoir under the scalp during surgery. The doctor injects drugs into the device. This method usually doesn’t hurt. The doctor may suggest this method when many doses of intrathecal chemotherapy are planned.
You may receive chemotherapy in a clinic, at the doctor’s office, or at home. Some people need to stay in the hospital during treatment.
Ask whether chemotherapy could make you unable to have children. Chemotherapy can cause infertility in adults, but most children treated with chemotherapy for leukemia seem to have normal fertility when they grow up. If teens or adults want to have a child someday after treatment, they may choose to store sperm or eggs before treatment starts.
Targeted therapy
Targeted therapies are drugs that can block the growth of leukemia cells. For example, a targeted therapy may block the action of an abnormal protein that causes leukemia cells to grow.
Several targeted therapies are used for leukemia. The type of targeted therapy depends on the type of leukemia:
- item__For CML and ALL: People with the Philadelphia chromosome may receive a targeted therapy. Nearly everyone with CML (chronic myeloid leukemia) and some people with ALL (acute lymphocytic
leukemia) have this chromosome. The targeted therapy used for CML and ALL is a pill that you swallow. Possible side effects include nausea, diarrhea, rash, and swelling. This drug may also cause headache, hair loss, or joint pain.
- item__For CLL: People who have CLL (chronic lymphocytic leukemia) may receive a targeted therapy that is different from the one used for CML and ALL. This drug is given directly into a vein through a thin needle. It may cause nausea, vomiting, diarrhea, night sweats, or joint pain. Side effects usually go away after treatment ends.
Radiation therapy
Some people with leukemia receive radiation therapy along with chemotherapy. You’ll lie down on a treatment table, and a large machine will aim high-energy rays at your body to kill cancer cells. The machine may be aimed at the brain or other parts of the body where leukemia cells have been found. Or, the machine may be aimed at the whole body.
You’ll go to a hospital or clinic for treatment. Radiation therapy for the brain or other areas is usually given 5 days a week for several weeks. Radiation therapy for the whole body is given once or twice a day for a few days, usually before a stem cell transplant.
Stem cell transplant
Some people with leukemia receive a stem cell transplant. This treatment is done after radiation therapy aimed at the whole body, a large dose of chemotherapy, or both. Radiation therapy and chemotherapy will destroy both leukemia cells and normal blood stem cells in the bone marrow.
Stem cell transplants take place in the hospital. You may need to stay in the hospital for several weeks.
To replace the normal blood stem cells that are destroyed by radiation therapy and chemotherapy, you’ll receive healthy blood stem cells through a vein. It’s like getting a blood transfusion. The transplanted stem cells will move to the bone marrow and make new blood cells.
Leukemia related genes
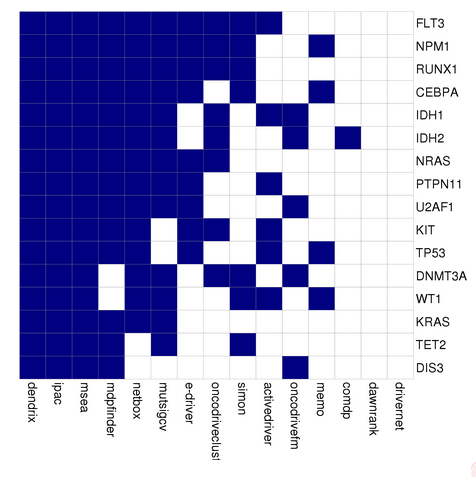
Leukemia Drugs
Leukemia Clinical Trials
You can ask your doctor to help you find a clinical trial, what’s involved, and what to consider -- for instance, if you’d need to travel to take part. You can also check these websites for information.
Eviti Clinical Trials
This website, developed by the nonprofit Coalition of Cancer Cooperative Groups, is the leading cancer clinical trial search engine. You can search for cancer trials based on disease and location.
National Cancer Institute
This website lists more than 6,000 cancer clinical trials and explains what to do when you find one that you think is right for you.
ClinicalTrials.gov
This website, a service of the National Institutes of Health, is a database of clinical studies worldwide.
CenterWatch
This web site lists industry-sponsored clinical trials that are recruiting patients.
Side Effects
Chemotherapy
The side effects depend mainly on which drugs are given and how much. Chemotherapy kills fast-growing leukemia cells, but the drugs can also harm normal cells that divide rapidly:
- item__Blood cells: When drugs lower the levels of healthy blood cells, you’re more likely to get infections, bruise or bleed easily, and feel very weak and tired. Your health care team will check for low levels of blood cells. If your levels are low, your health care team may stop the chemotherapy for a while, reduce the dose of the drug, or give you a blood transfusion. They may also give you medicines that help your body to make new blood cells.
- item__leukemia) have this chromosome. The targeted therapy used for CML and ALL is a pill that you swallow. Possible side effects include nausea, diarrhea, rash, and swelling. This drug may also cause headache, hair loss, or joint pain.
- item__For CLL: People who have CLL (chronic lymphocytic leukemia) may receive a targeted therapy that is different from the one used for CML and ALL. This drug is given directly into a vein through a thin needle. It may cause nausea, vomiting, diarrhea, night sweats, or joint pain. Side effects usually go away after treatment ends.
Radiation Therapy
Side effects depend mainly on how much radiation is given and the part of your body that is treated. Ask your health care team what to expect. Side effects may develop during radiation therapy or months or years later.
Radiation therapy aimed at the brain may cause you to feel tired or to lose hair from your head. Your health care team can suggest ways to manage these problems, which usually go away when treatment ends. However, some side effects, such as memory loss or other problems, may be permanent.
It’s common for skin in the treated area to become red, dry, and itchy. Check with your doctor before using lotion or cream on that area. After treatment is over, the skin will slowly heal.
You’re likely to become tired during radiation therapy, especially in the later weeks of treatment. Although getting enough rest is important, most people say they feel better when they exercise every day. Try to go for a short walk, do gentle stretches, or do yoga.
Nutrition of the patients
Eating well is important before, during, and after treatment for leukemia. You need the right amount of calories to maintain a good weight. You also need enough protein to keep up your strength. Eating well may help you feel better and have more energy.
Sometimes, especially during or soon after treatment, you may not feel like eating. You may be uncomfortable or tired. You may find that foods don’t taste as good as they used to. In addition, poor appetite, nausea, vomiting, mouth blisters, and other side effects of treatment can make it hard for you to eat.
Follow-up Care
After treatment for leukemia, you’ll need regular checkups. For example, someone with acute leukemia may need a checkup every month for the first year after treatment, and someone with chronic leukemia may need a checkup every six months.
Checkups help ensure that any changes in your health are noted and treated if needed. If you have any health problems between checkups, contact your doctor.
Leukemia may come back after treatment. Your doctor will check for the return of leukemia. Checkups also help detect health problems that can result from cancer treatment.
Checkups may include a physical exam, blood tests, and bone marrow tests.