Hepatobiliary cancer
Hepatobiliary cancer
What is Hepatobiliary cancer
Hepatobiliary cancer is a kind of liver cancer. Liver cancer is cancer that begins in the cells of your liver. Your liver is a football-sized organ that sits in the upper right portion of your abdomen, beneath your diaphragm and above your stomach.
Primary liver cancer is globally the sixth most frequent cancer (6%) and the second leading cause of death from cancer (9%).In 2012 it occurred in 782,000 people and in 2015 resulted in 810,500 deaths. In 2015, 263,000 deaths from liver cancer were due to hepatitis B, 167,000 to hepatitis C, and 245,000 to alcohol. Higher rates of liver cancer occur where hepatitis B and C are common, including Asia and sub-Saharan Africa.Males are more often affected with HCC than females.[3] Diagnosis is most frequent among those 55 to 65 years old. Five-year survival rates are 18% in the United States.The word "hepatic" is from the Greek hêpar, meaning "liver."
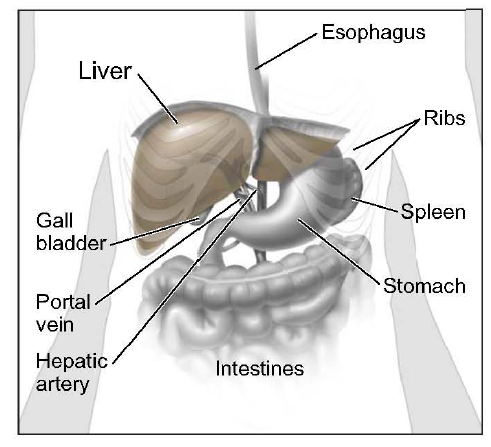
Types of Hepatobiliary cancer
Several types of cancer can form in the liver. The most common type of liver cancer is hepatocellular carcinoma, which begins in the main type of liver cell (hepatocyte). Other types of liver cancer, such as intrahepatic cholangiocarcinoma and hepatoblastoma, are much less common.
Not all cancers that affect the liver are considered liver cancer. Cancer that begins in another area of the body — such as the colon, lung or breast — and then spreads to the liver is called metastatic cancer rather than liver cancer. And this type of cancer is named after the organ in which it began — such as metastatic colon cancer to describe cancer that begins in the colon and spreads to the liver. Cancer that spreads to the liver is more common than cancer that begins in the liver cells.
Risk factor of Hepatobiliary cancer
Factors that increase the risk of primary liver cancer include:
Chronic infection with HBV or HCV.
Chronic infection with the hepatitis B virus (HBV) or hepatitis C virus (HCV) increases your risk of liver cancer.
Cirrhosis.
This progressive and irreversible condition causes scar tissue to form in your liver and increases your chances of developing liver cancer.
Certain inherited liver diseases.
Liver diseases that can increase the risk of liver cancer include hemochromatosis and Wilson's disease.
Diabetes.
People with this blood sugar disorder have a greater risk of liver cancer than those who don't have diabetes.
Nonalcoholic fatty liver disease.
An accumulation of fat in the liver increases the risk of liver cancer.
Exposure to aflatoxins.
Aflatoxins are poisons produced by molds that grow on crops that are stored poorly. Crops such as corn and peanuts can become contaminated with aflatoxins, which can end up in foods made of these products. In the United States, safety regulations limit aflatoxin contamination. Aflatoxin contamination is more common in certain parts of Africa and Asia.
Excessive alcohol consumption.
Consuming more than a moderate amount of alcohol daily over many years can lead to irreversible liver damage and increase your risk of liver cancer.
Symptoms of Hepatobiliary cancer
Most people don't have signs and symptoms in the early stages of primary liver cancer. When signs and symptoms do appear, they may include:
- item Losing weight without trying
- item Loss of appetite
- item Upper abdominal pain
- item Nausea and vomiting
- item General weakness and fatigue
- item Abdominal swelling
- item Yellow discoloration of your skin and the whites of your eyes (jaundice)
- item White, chalky stools
Diagnosis & Tests
Hepatocellular carcinoma (HCC) is the most common type of primary liver cancer. Hepatocellular carcinoma occurs most often in people with chronic liver diseases, such as cirrhosis caused by hepatitis B or hepatitis C infection.
Tests and procedures used to diagnose hepatocellular carcinoma include:
- item Blood tests to measure liver function
- item Imaging tests, such as CT and MRI with contrast, and advanced imaging procedures, such as magnetic resonance elastography
- item Liver biopsy, in some cases, to remove a sample of liver tissue for laboratory testing
Stage of Hepatobiliary cancer
Treatment
Which treatment is best for you will depend on the size and location of your hepatocellular carcinoma, how well your liver is functioning, and your overall health.
Hepatocellular carcinoma treatments include:
- item Surgery. Surgery to remove the cancer and a margin of healthy tissue that surrounds it may be an option for people with early-stage liver cancers who have normal liver function.
- item Liver transplant surgery. Surgery to remove the entire liver and replace it with a liver from a donor may be an option in otherwise healthy people whose liver cancer hasn't spread beyond the liver.
- item Destroying cancer cells with heat or cold. Ablation procedures to kill the cancer cells in the liver using extreme heat or cold may be recommended for people who can't undergo surgery. These procedures include radiofrequency ablation, cryoablation, and ablation using alcohol or microwaves.
- item Delivering chemotherapy or radiation directly to cancer cells. Using a catheter that's passed through your blood vessels and into your liver, doctors can deliver chemotherapy drugs (chemoembolization) or tiny glass spheres containing radiation (radioembolization) directly to the cancer cells.
- item Targeted drug therapy. Targeted drugs, such as sorafenib (Nexavar), may help slow the progression of the disease in people with advanced liver cancer.
- item Radiation therapy. Radiation therapy using energy from X-rays or protons may be recommended if surgery isn't an option. A specialized type of radiation therapy, called stereotactic body radiotherapy (SBRT), involves focusing many beams of radiation simultaneously at one point in your body.
Hepatobiliary cancer related genes
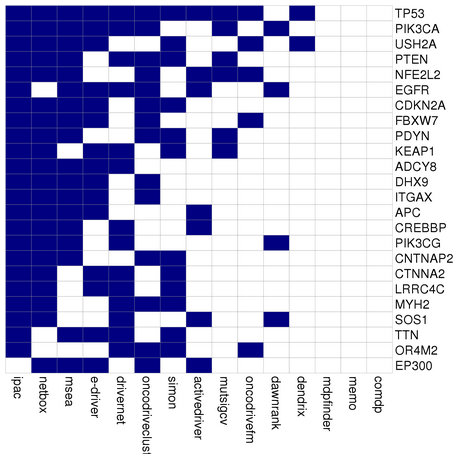
Hepatobiliary cancer Drugs
Hepatobiliary cancer Clinical Trials
Clinical trials are a way to try new medications and treatments that researchers are testing. The goal is to find out how well these treatments work and what side effects they could have.
People with breast cancer who participate in cancer clinical trials get the most effective therapy that’s already available, or they may receive new cancer treatments that are being tested for future use.
You can ask your doctor to help you find a clinical trial, what’s involved, and what to consider -- for instance, if you’d need to travel to take part. You can also check these websites for information.
Eviti Clinical Trials
This website, developed by the nonprofit Coalition of Cancer Cooperative Groups, is the leading cancer clinical trial search engine. You can search for cancer trials based on disease and location.
Eviti Clinical Trials
This website, developed by the nonprofit Coalition of Cancer Cooperative Groups, is the leading cancer clinical trial search engine. You can search for cancer trials based on disease and location.
National Cancer Institute
This website lists more than 6,000 cancer clinical trials and explains what to do when you find one that you think is right for you.
ClinicalTrials.gov
This website, a service of the National Institutes of Health, is a database of clinical studies worldwide.
CenterWatch
This web site lists industry-sponsored clinical trials that are recruiting patients.
Side Effects
Surgery
Pain and weakness. Your doctor will prescribe medication to relieve your pain, but you’ll need to allow time to rest and heal. It’s a good idea to keep a journal so you can track and describe your symptoms. If it gets worse, work with your doctor to adjust medications and fine-tune the dosage.
Chemotherapy
Shortness of breath. You may feel this even though you’re getting enough oxygen and you can breathe normally. It’s how your brain processes chest pain. It should get better over the next few weeks as you heal. If your breast are in good shape (other than the cancer) you can usually return to normal life after a while -- even if an entire breast was removed. If you also have a non-cancerous disease like emphysema or chronic bronchitis, you may always feel short of breath with some types of activity.
Nausea and vomiting. Feeling like you're going to throw up or actually doing it can be a problem on treatment days. Your doctor will give you medicine to keep these symptoms at bay.
Hair loss. Follicles, the tiny structures that hair grows out of, contain some of the fastest-growing cells in your body. So chemo attacks them, too. Within a few weeks of starting treatment, you may lose some or all of your hair. The good news is that it's almost always temporary. It can make you feel better to cut or shave before it starts to fall out. If you opt to go bald, use an electric shaver so you don't cut your scalp. If you get a wig, shop for it while you still have hair so you can match it to your current hair color.
Bleeding or clotting problems. Platelets are blood cells that help stop bleeding. They plug damaged blood vessels and help your blood clot. If you don't have enough of them, you may bleed or bruise more easily than usual, even from a minor injury. Your doctor will check your platelet count often during your treatment. If it falls too low, you may need a transfusion.
Loss of appetite. Instead of three large meals per day, have five or six small ones. Avoid greasy, salty, sweet, or spicy food that might make you feel queasy. If even the smell of food is a turnoff, eat cold meals instead.
Diarrhea. Frequent bowel movements that are loose or watery can get in the way of your daily life. They can also drain too much liquid from your body. Skip dairy and high-fiber, greasy, or spicy foods. Drink water or suck on ice chips, and call you doctor if your symptoms last more than a day.
Nutrition of the patients
Eating well is important before, during, and after cancer treatment. You need the right amount of calories to maintain a good weight. You also need enough protein to keep up your strength. Eating well may help you feel better and have more energy.
Sometimes, especially during or soon after treatment, you may not feel like eating. You may be uncomfortable or tired. You may find that foods don’t taste as good as they used to. In addition, poor appetite, nausea, vomiting, mouth blisters, and other side effects of treatment can make it hard for you to eat.
Your doctor, a registered dietitian, or another health care provider can suggest ways to help you meet your nutrition needs.
Follow-up Care
You’ll need regular checkups (such as every 6 months) after treatment for lung cancer. Checkups help ensure that any changes in your health are noted and treated if needed. If you have any health problems between checkups, contact your doctor.
Lung cancer may come back after treatment. Your doctor will check for the return of cancer. It may return in the chest or it may return in another part of the body, such as the bones.
Checkups also help detect health problems that can result from cancer treatment.
Checkups may include a physical exam, blood tests, or CT scans.