Pancreatic cancer
Pancreatic cancer
What is Pancreatic cancer
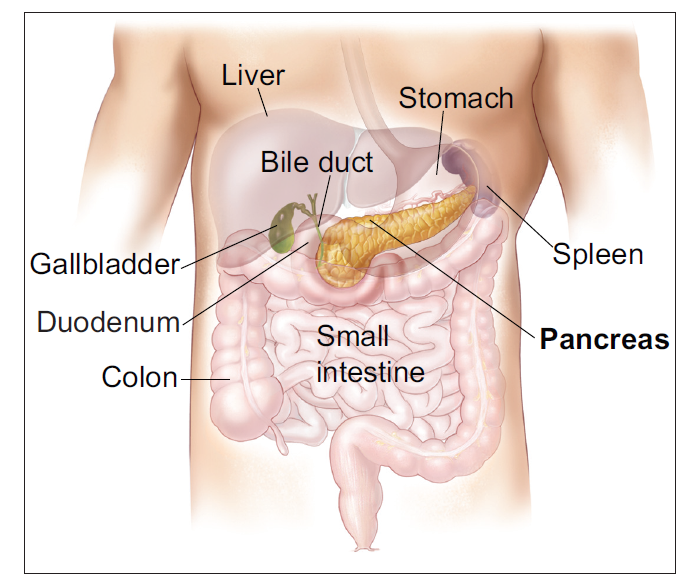
The pancreas is an organ that is about 6 inches long. It’s located deep in your belly between your stomach and backbone. Your liver, intestine, and other organs surround your pancreas.
The widest part of the pancreas is called the head. The head of the pancreas is closest to the small intestine. The middle section is called the body, and the thinnest part is called the tail.
The pancreas makes pancreatic juices. These juices contain enzymes that help break down food. The juices flow through a system of ducts leading to the main pancreatic duct. The pancreatic juices flow through the main duct to the duodenum, the first part of the small intestine.
The pancreas is also a gland that makes insulin and other hormones. These hormones enter the bloodstream and travel throughout the body. They help the body use or store the energy that comes from food. For example, insulin helps control the amount of sugar in the blood. Cancer begins in cells, the building blocks that make up tissues. Tissues make up the pancreas and the other organs of the body.
Normal cells grow and divide to form new cells as the body needs them. When normal cells grow old or get damaged, they die, and new cells take their place. Sometimes, this process goes wrong. New cells form when the body doesn’t need them, and old or damaged cells don’t die as they should. The buildup of extra cells often forms a mass of tissue called a growth or tumor.
Tumors in the pancreas can be benign (not cancer) or malignant (cancer). Benign tumors are not as harmful as malignant tumors:
Benign tumors
- item Are rarely a threat to life
- item Don’t invade the tissues around them
- item Don’t spread to other parts of the body
- item Usually don’t need to be removed
Malignant tumors
- item May be a threat to life
- item Can invade nearby organs and tissues
- item Can spread to other parts of the body
- item Often can be removed but may grow back
Types of Pancreatic cancer
Pancreatic cancer can invade other tissues, shed cancer cells into the abdomen, or spread to other organs:
- item__Invade: A malignant pancreatic tumor can grow and invade organs next to the pancreas, such as the stomach or small intestine.
- Item__Shed: Cancer cells can shed (break off) from the main pancreatic tumor. Shedding into the abdomen may lead to new tumors forming on the surface of nearby organs and tissues. The doctor may call these seeds or implants. The seeds can cause an abnormal buildup of fluid in the abdomen (ascites).
- Item__Spread: Cancer cells can spread by breaking away from the original tumor. They can spread through the blood vessels to the liver and lungs. In addition, pancreatic cancer cells can spread through lymph vessels to nearby lymph nodes. After spreading, the cancer cells may attach to other tissues and grow to form new tumors that may damage those tissues.
Molecular classification
Risk factor of Pancreatic cancer
When you get a diagnosis of cancer, it’s natural to wonder what may have caused the disease. Doctors can’t always explain why one person gets pancreatic cancer and another doesn’t. However, we do know that people with certain risk factors may be more likely than others to develop cancer of the pancreas. A risk factor is something that may increase the chance of getting a disease.
Studies have found the following risk factors for cancer of the pancreas:
- item Smoking: Smoking tobacco is the most important risk factor for pancreatic cancer. People who smoke tobacco are more likely than nonsmokers to develop this disease. Heavy smokers are most at risk.
- item Diabetes: People with diabetes are more likely than ther people to develop pancreatic cancer.
- item Family history: Having a mother, father, sister, or brother with pancreatic cancer increases the risk of developing the disease.
- item Inflammation of the pancreas: Pancreatitis is a painful inflammation of the pancreas. Having pancreatitis for a long time may increase the risk of pancreatic cancer.
- item Obesity: People who are overweight or obese are slightly more likely than other people to develop pancreatic cancer. Many other possible risk factors are under active study. For example, researchers are studying whether a diet high in fat (especially animal fat) or heavy drinking of alcoholic beverages may increase the risk of pancreatic cancer. Another area of active research is whether certain genes increase the risk of disease. Many people who get pancreatic cancer have none of these risk factors, and many people who have known risk factors don’t develop the disease.
Symptoms of Pancreatic cancer
Early cancer of the pancreas often doesn’t cause symptoms. When the cancer grows larger, you may notice one or more of these common symptoms:
- item Dark urine, pale stools, and yellow skin and eyes from jaundice
- item Pain in the upper part of your belly
- item Pain in the middle part of your back that doesn’t go away when you shift your position
- item Nausea and vomiting
- item Stools that float in the toilet Also, advanced cancer may cause these general symptoms:
- item Weakness or feeling very tired
- item Loss of appetite or feelings of fullness
- item Weight loss for no known reason
- item These symptoms may be caused by pancreatic cancer or by other health problems. People with these symptoms should tell their doctor so that problems can be diagnosed and treated as early as possible
Diagnosis & Tests
If you have symptoms that suggest cancer of the pancreas, your doctor will try to find out what’s causing the problems. You may have blood or other lab tests. Also, you may have one or more of the following tests:
- item Physical exam: Your doctor feels your abdomen to check for changes in areas near the pancreas, liver, gallbladder, and spleen. Your doctor also checks for an abnormal buildup of fluid in the abdomen. Also, your skin and eyes may be checked for signs of jaundice.
- item CT scan: An x-ray machine linked to a computer takes a series of detailed pictures of your pancreas, nearby organs, and blood vessels in your abdomen. You may receive an injection of contrast material so your pancreas shows up clearly in the pictures. Also, you may be asked to drink water so your stomach and duodenum show up better. On the CT scan, your doctor may see a tumor in the pancreas or elsewhere in the abdomen.
- item Ultrasound: Your doctor places the ultrasound device on your abdomen and slowly moves it around. The ultrasound device uses sound waves that can’t be heard by humans. The sound waves make a pattern of echoes as they bounce off internal organs. The echoes create a picture of your pancreas and other organs in the abdomen. The picture may show a tumor or blocked ducts.
- item EUS: Your doctor passes a thin, lighted tube (endoscope) down your throat, through your stomach, and into the first part of the small intestine. An ultrasound probe at the end of the tube sends out sound waves that you can’t hear. The waves bounce off tissues in your pancreas and other organs. As your doctor slowly withdraws the probe from the intestine toward the stomach, the computer creates a picture of the pancreas from the echoes. The picture can show a tumor in the pancreas. It can also show how deeply the cancer has invaded the blood vessels. Some doctors use the following tests also:
- item ERCP: The doctor passes an endoscope through your mouth and stomach, down into the first part of your small intestine. Your doctor slips a smaller tube through the endoscope into the bile ducts and pancreatic ducts. After injecting dye through the smaller tube into the ducts, the doctor takes x-ray pictures. The x-rays can show whether the ducts are narrowed or blocked by a tumor or other condition.
- item MRI: A large machine with a strong magnet linked to a computer is used to make detailed pictures of areas inside your body.
- item PET scan: You’ll receive an injection of a small amount of radioactive sugar. The radioactive sugar gives off signals that the PET scanner picks up. The PET scanner makes a picture of the places in your body where the sugar is being taken up. Cancer cells show up brighter in the picture because they take up sugar faster than normal cells do. A PET scan may show a tumor in the pancreas. It can also show cancer that has spread to other parts of the body.
- item Needle biopsy: The doctor uses a thin needle to remove a small sample of tissue from the pancreas. EUS or CT may be used to guide the needle. A pathologist uses a microscope to look for cancer cells in the tissue.
Stage of Pancreatic cancer
If cancer of the pancreas is diagnosed, your doctor needs to learn the extent (stage) of the disease to help you choose the best treatment.
When cancer of the pancreas spreads, the cancer cells may be found in nearby lymph nodes or the liver. Cancer cells may also be found in the lungs or in fluid collected from the abdomen.
When cancer spreads from its original place to another part of the body, the new tumor has the same kind of abnormal cells and the same name as the original (primary) tumor. For example, if pancreatic cancer spreads to the liver, the cancer cells in the liver are actually pancreatic cancer cells. The disease is metastatic pancreatic cancer, not liver cancer. It’s
treated as pancreatic cancer, not as liver cancer. Doctors sometimes call the new tumor in the liver “distant" disease.
To learn whether pancreatic cancer has spread, your doctor may order CT scans or EUS.
Also, a surgeon may look inside your abdomen with a laparoscope (a thin, tube-like device that has a light and a lens for seeing inside the body). The surgeon inserts the laparoscope through a small incision in your belly button. The surgeon will look for any signs of cancer inside your abdomen. You’ll need general anesthesia for this exam.
These are the stages of cancer of the pancreas:
- item Stage I: The tumor is found only in the pancreas.
- item The cancer may have spread to the lymph nodes.
- item Stage III: The tumor has invaded nearby blood vessels.
- item Stage IV: The cancer has spread to a distant organ, such as the liver or lungs.
Treatment
Surgery
Surgery may be an option for people with an early stage of pancreatic cancer. The surgeon usually removes only the part of the pancreas that has cancer.
But, in some cases, the whole pancreas may beremoved.
The type of surgery depends on the location of thetumor in the pancreas. Surgery to remove a tumor in the head of the pancreas is called a Whipple procedure.
The Whipple procedure is the most common type of surgery for pancreatic cancer. You and your surgeon may talk about the types of surgery and which may be right for you.
In addition to part or all of your pancreas, the surgeon usually removes the following nearby tissues:
- item Duodenum
- item Gallbladder
- item Common bile duct
- item Part of your stomach
Also, the surgeon may remove your spleen and nearby lymph nodes. Surgery for pancreatic cancer is a major operation. You will need to stay in the hospital for one to two weeks afterward. Your health care team will watch for signs of bleeding, infection, or other problems. It takes time to heal after surgery, and the time needed to recover is different for each person. You may have pain or discomfort for the first few days.
Medicine can help control your pain. Before surgery, you should discuss the plan for pain relief with your health care team. After surgery, they can adjust the plan if you need more pain control.
It’s common to feel weak or tired for a while. You may need to rest at home for one to three months after leaving the hospital.
After surgery, it may be hard to digest food. For four to six weeks after Whipple surgery, you may feel bloated or full, and you may have nausea and vomiting. A dietitian can help you change your diet to reduce your discomfort. Problems with eating usually go away within three months.
Chemotherapy
Chemotherapy uses drugs to kill cancer cells. Most people with pancreatic cancer get chemotherapy. For early pancreatic cancer, chemotherapy is usually given after surgery, but in some cases, it’s given before surgery. For advanced cancer, chemotherapy is used alone, with targeted therapy, or with radiation therapy. Chemotherapy for pancreatic cancer is usually given by vein (intravenous). The drugs enter the bloodstream and travel throughout your body. Chemotherapy may be given in an outpatient part of the hospital, at the doctor’s office, or at home. Rarely, you may need to stay in the hospital.
Targeted Therapy
People with cancer of the pancreas who can’t have surgery may receive a type of drug called targeted therapy along with chemotherapy.
Targeted therapy slows the growth of pancreatic cancer. It also helps prevent cancer cells from spreading. The drug is taken by mouth.
Radiation Therapy
Radiation therapy uses high-energy rays to kill cancer cells. It can be given along with other
treatments, including chemotherapy. The radiation comes from a large machine. The machine aims beams of radiation at the cancer in the abdomen. You’ll go to a hospital or clinic 5 days a week for several weeks to receive radiation therapy.
Each session takes about 30 minutes.
Pancreatic cancer related genes
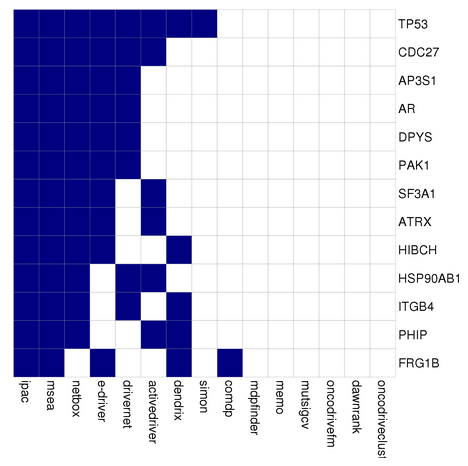
Pancreatic cancer Drugs
Pancreatic cancer Clinical Trials
You can ask your doctor to help you find a clinical trial, what’s involved, and what to consider -- for instance, if you’d need to travel to take part. You can also check these websites for information.
Eviti Clinical Trials
This website, developed by the nonprofit Coalition of Cancer Cooperative Groups, is the leading cancer clinical trial search engine. You can search for cancer trials based on disease and location.
National Cancer Institute
This website lists more than 6,000 cancer clinical trials and explains what to do when you find one that you think is right for you.
ClinicalTrials.gov
This website, a service of the National Institutes of Health, is a database of clinical studies worldwide.
CenterWatch
This web site lists industry-sponsored clinical trials that are recruiting patients.
Side Effects
Radiation Therapy
Although radiation therapy is painless, it may cause other side effects. The side effects include nausea, vomiting, or diarrhea. You may also feel very tired.
Your health care team can suggest ways to treat or control these side effects.
Nutrition of the patients
Nutrition is an important part of your care. Getting the right nutrition can help you feel better and have more strength. However, pancreatic cancer and its treatment may make it hard for you to digest food and to maintain your weight. You may not feel like eating for a variety of reasons, such as feeling tired or feeling full soon after eating.
You may find it helpful to work with a dietitian. A dietitian can help you choose foods and nutrition products that will meet your needs and can make you feel more comfortable with eating. Your health care team will check you for weight loss and ask whether you are having problems with nausea, vomiting, or diarrhea. If your nutrition problems do not get better quickly enough, you may be offered another way of getting nutrition, such as a feeding tube.
After surgery, your health care team will check you for problems with digestion or with your blood sugar level, and they will help you manage such changes. If you have problems with digestion, you may need to take a supplement to replace the digestive enzymes that are normally made by the pancreas. You may also need to take minerals and vitamins. If you have problems with the sugar level in your blood, you may need to take medicine to control blood sugar.
Follow-up Care
You’ll need regular checkups (such as every 3 months) after treatment for cancer of the pancreas. Checkups help ensure that any changes in your health are noted and treated if needed. If you have any health problems between checkups, you should contact your
doctor. Cancer of the pancreas may come back after treatment. Your doctor will check for return of cancer. Checkups may include a physical exam, blood tests, or CT scans.